Lumbar Stenosis
Stenosis is characterised by leg pain or symptoms of neurological or vascular compromise in one or both legs related to prolonged standing and/or walking. Symptoms are usually relieved quite quickly when the patient sits down.
Anatomy
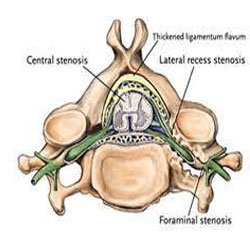
Stenosis occurs when there is a functional decrease in cross-sectional area within either one or more lumbar spine foraminal spaces or centrally within the spinal canal itself. This decrease in cross-sectional area compresses the neurovascular bundles that are contained within these spaces. The size of the space is usually decreased by a space occupying lesion such as a posterior central disc bulge, a postero-lateral disc bulge (the foramen is compromised), arthritic facet joints with large osteophytes protruding into the foramen, a spondylolisthesis, or the neurovascular bundle can functionally be irritated by an increase in chemical inflammation and the resulting increase in local pressure can block mobility within the small spaces.
Why does standing and walking cause the most problems?
The symptoms are aggravated by standing and walking activities as these movements functionally close down of the foramen (of most commonly the L5S1 segment), which in turn compresses the structures that pass through the foramen. Walking and standing also extends the lower lumbar spine which increases central compression if there is a central canal stenosis present.
Physiotherapy Treatment
Physiotherapy treatment can be highly effective to relieve the symptoms of stenosis and can include lumbar rotation mobilisations (to open the foramen), straight leg raise stretches (to stretch the affected tissues), hydrotherapy for mobility and fitness, and a home exercise program to maintain flexibility and movement and improve muscle strength and control. Patient education is also essential to assist in the recovery of function. If the patient can learn to self manage the condition and decrease the potential for aggravation, there is a much greater chance of conservative management being all that is required.

